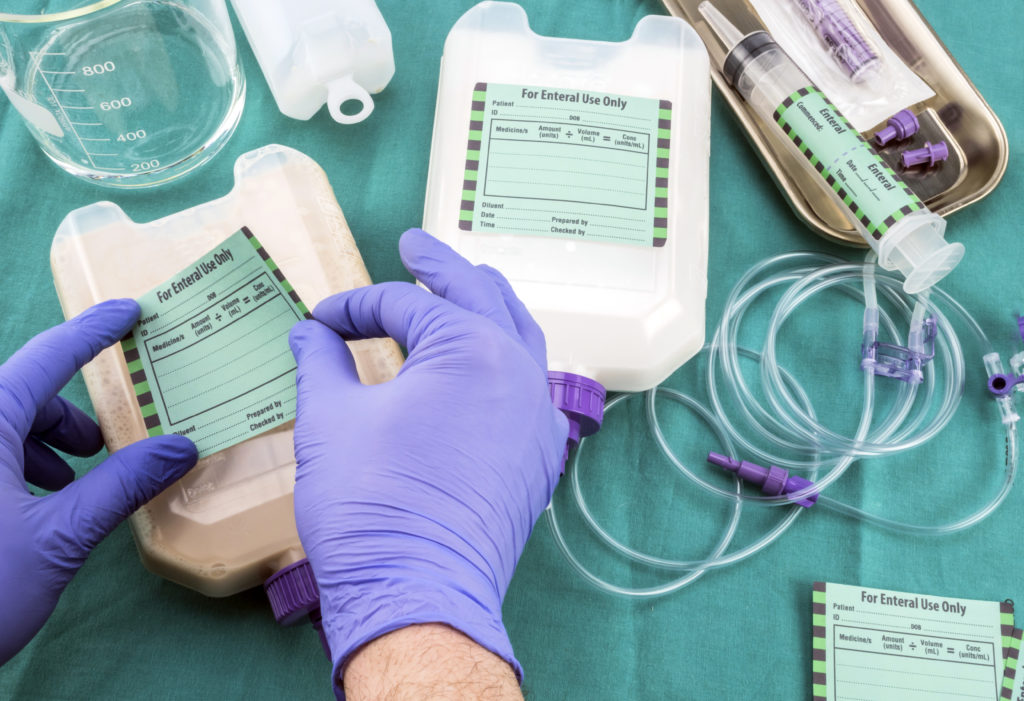
When illness, injury, or certain medical conditions prevent individuals from consuming a regular diet, alternative methods of providing nutrition become essential. Enteral nutrition, also known as tube feeding, is a method of delivering nutrition directly into the gastrointestinal tract. Enteral nutrition involves the delivery of a nutritionally complete liquid formula through a tube that is inserted into the stomach or small intestine. This method allows individuals who are unable to eat or have difficulty swallowing to receive the essential nutrients they need for sustenance and recovery. It is commonly used in hospitals, long-term care facilities, and home care settings to support patients with various medical conditions.
There are several indications for enteral nutrition. It is frequently employed in patients who have undergone surgery, particularly those undergoing gastrointestinal procedures or those unable to consume food orally in the immediate postoperative period. Patients with conditions such as cancer, severe malnutrition, neurological disorders, or gastrointestinal disorders that impair nutrient absorption may also require Enteral Nutrition. Additionally, individuals with impaired swallowing function, such as those with stroke, head and neck cancer, or neurological deficits, may benefit from this method of nutrition delivery.
The global Enteral Nutrition Market is estimated to be valued at US$ 2,635.9 million in 2020 and is expected to exhibit a CAGR of 5.8% over the forecast period (2020-2027).
One of the primary advantages of enteral nutrition is that it allows for the provision of a balanced and tailored nutritional formula that meets the specific needs of the individual. These formulas are designed to provide carbohydrates, proteins, fats, vitamins, minerals, and other essential nutrients in the appropriate proportions. They can be adjusted based on the patient’s age, weight, medical condition, and nutrient requirements. The formulas come in various forms, including ready-to-use liquid formulas, powders, or modular components that can be mixed with water.
Enteral nutrition offers numerous benefits beyond meeting nutritional needs. It helps maintain the structure and function of the gastrointestinal tract, as it continues to receive stimulation from the feeding. This stimulation promotes gut health and integrity, preventing complications such as bacterial overgrowth or translocation. Additionally, enteral feeding can reduce the risk of malnutrition, maintain muscle mass, support wound healing, and improve immune function, leading to better overall patient outcomes.
Implementing Enteral Nutrition requires a multidisciplinary approach. A team of healthcare professionals, including physicians, dietitians, nurses, and pharmacists, collaborates to determine the most appropriate feeding method, formula selection, and tube placement. Various routes can be used for tube insertion, including nasogastric, nasoenteric, or gastrostomy tubes. The selection of the appropriate route depends on the patient’s condition, expected duration of feeding, and anticipated complications.
Proper care and management of the feeding tube are essential to prevent complications. Regular monitoring of tube placement, gastric residual volumes, and signs of intolerance or infection is necessary. The healthcare team ensures that the feeding tube remains secure, functional, and free from blockages. They also provide ongoing education and support to the patient and caregivers on tube care, administration techniques, and recognizing potential complications.
Enteral nutrition can be administered in various ways, depending on the patient’s condition and requirements. Continuous feeding involves a slow and steady infusion of the formula over a set period, usually 24 hours. This method is commonly used in critically ill patients or those with compromised digestion or absorption. Intermittent feeding, on the other hand, involves delivering larger volumes of the formula several times a day, usually over 30 minutes to 2 hours. This method is suitable for patients with a functioning gastrointestinal tract who can tolerate larger volumes of feeding at once.
Transitioning from enteral nutrition to oral intake is a crucial goal for many patients. As the patient’s condition improves, the healthcare team gradually introduces oral intake while reducing the volume of enteral feeding. Close monitoring and individualized adjustments are made to ensure a smooth transition and prevent complications.